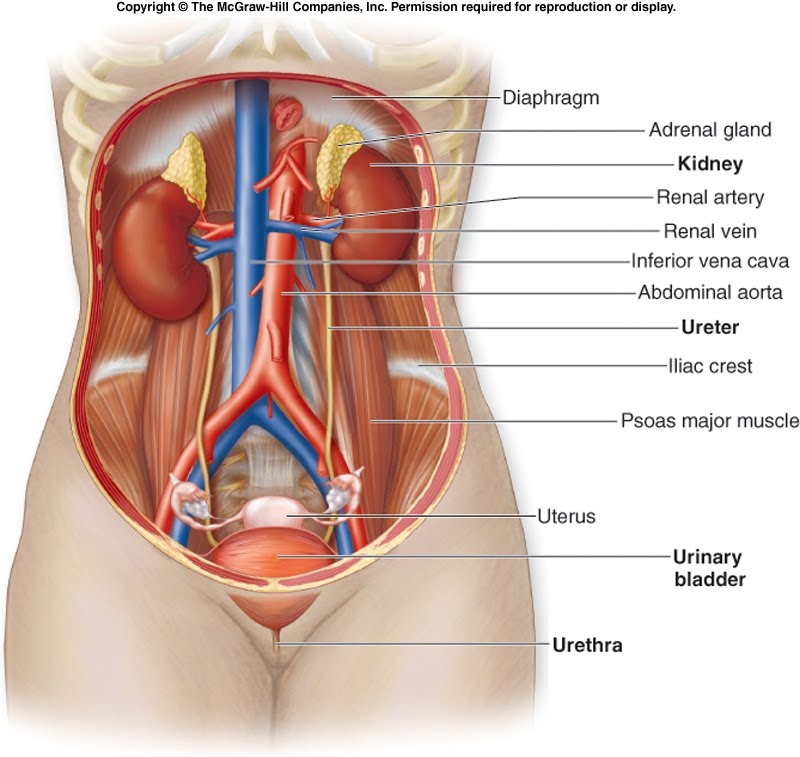
Chronic kidney disease (CKD) is a progressive loss in kidney function over a period of months or years. Each of your kidneys has about a million tiny filters, called nephrons. If nephrons are damaged, they stop working. For a while, healthy nephrons can take on the extra work. But if the damage continues, more and more nephrons shut down. After a certain point, the nephrons that are left cannot filter your blood well enough to keep you healthy.
When kidney function falls below a certain point, it is called kidney failure. Kidney failure affects your whole body, and can make you feel very ill. Untreated kidney failure can be life-threatening.
Common: Between 8 and 10% of the adult population have some form of kidney damage, and every year millions die prematurely of complications related to Chronic Kidney Diseases (CKD).
Harmful:
Treatable: If CKD is detected early and managed appropriately, the deterioration in kidney function can be slowed or even stopped, and the risk of associated cardiovascular complications can be reduced.
How is kidney function measured?
The main indicator of kidney function is your blood level of creatinine, a waste product of the body produced by muscles and excreted by the kidneys. If kidney function is reduced, creatinine accumulates in the blood leading to an elevated level when a blood test is checked.
Kidney function is best measured by an indicator called GFR (Glomerular Filtration Rate) which measures the blood filtration rate by kidneys. This indicator allows doctors to determine if the kidney function is normal, and if not, to what level the reduced kidney function has deteriorated. In everyday practice, GFR can easily be estimated (eGFR), from measurement of the blood creatinine level, and taking into account, age, ethnicity and gender.
Stages of Chronic Kidney Disease (CKD)
Usually, kidney disease starts slowly and silently, and progresses over a number of years. Not everyone progresses from Stage 1 to Stage 5. Stage 5 is also known as End-Stage Renal Disease (ESRD).
|
Stage |
Description |
GFR Level |
|
Normal Kidney Function |
Healthy Kidneys |
90mL/min or more |
|
Stage 1 |
Kidney damage with normal or high GFR |
90ml/min or more |
|
Stage 2 |
Kidney damage and mild decrease in GFR |
60 to 89mL/min |
|
Stage 3 |
Moderate decrease in GFR |
30 to 59mL/min |
|
Stage 4 |
Severe decrease in GFR |
15 to 29 mL/min |
|
Stage 5 (ESKD) |
Established kidney failure |
Less than 15mL/min or on dialysis |
GFR: Glomerular Filtration Rate
CGA: Cause, GFR and Albuminuria categories
Source: “KDIGO 2012 Clinical Practice Guideline for the Evaluation and Management of Chronic Kidney Disease”.
Causes of CKD
High blood pressure (hypertension) and diabetes are the most common causes of kidney disease. The high blood pressure causes just over a quarter of all cases of kidney failure. Diabetes has been established as the cause of around one-third of all cases and is the commonest cause of ESRD in most developed countries.
Other less common conditions include inflammation (glomerulonephritis) or infections (pyelonephritis). Sometimes CKD is inherited (such as polycystic disease) or the result of longstanding blockage to the urinary system (such as enlarged prostate or kidney stones).
Some drugs can cause CKD, especially some pain-killing drugs (analgesics) if taken over a long time. Often doctors cannot determine what caused the problem.
Symptoms
A person can lose up to 90% of their kidney functions before experiencing any symptoms.
Most people have no symptoms until CKD is advanced. Signs of advancing CKD include swollen ankles, fatigue, difficulty concentrating, decreased appetite, blood in the urine and foamy urine.
Detection
The majority of individuals with early stages of CKD go undiagnosed. On WKD we are calling on everyone to check if they are at risk for kidney disease and encouraging people with any risk factors to take a simple kidney function test.
Kidney disease usually progresses silently, often destroying most of the kidney function before causing any symptoms. The early detection of failing kidney function is crucial because it allows suitable treatment before kidney damage or deterioration manifests itself through other complications.
Simple laboratory tests are done on small samples of blood (to measure creatinine content and estimate GFR) and on urine (to measure creatinine and albumin excretion).
Your doctor uses the results of your Serum Creatinine measured in the blood to estimate your overall kidney function, or Glomerular Filtration Rate (GFR) and your blood sugar to be sure you do not have diabetes. A simple “dipstick” test may be used to detect excess protein in the urine.
Treating CKD
There is no cure for chronic kidney disease, although treatment can slow or halt the progression of the disease and can prevent other serious conditions developing.
The main treatments are a proper diet and medications, and for those who reach ESRD, long term dialysis treatment or kidney transplantation. In the early stages of kidney disease, a proper diet and medications may help to maintain the critical balances in the body that your kidneys would normally control. However, when you have kidney failure, wastes and fluids accumulate in your body and you need dialysis treatments to remove these wastes and excess fluid from your blood, dialysis can be done either by machine (hemodialysis) or by using fluid in your abdomen (peritoneal dialysis). In suitable patients a kidney transplant combined with medications and a healthy diet can restore normal kidney function. Dialysis and kidney transplantation are known as renal replacement therapies (RRT) because they attempt to “replace” the normal functioning of the kidneys and are discussed in more detail below.
Kidney Transplantation
A kidney transplant is an operation to place a healthy (donor) kidney in your body to perform the functions your own diseased kidneys can no longer perform.
Kidney transplantation is considered the best treatment for many people with severe CKD because quality of life and survival are often better than in people who use dialysis. However, there is a shortage of organs available for donation. Many people who are candidates for kidney transplantation are put on a transplant waiting list and require dialysis until an organ is available.
A kidney can come from a living relative, a living unrelated person, or from a person who has died (deceased or cadaver donor); only one kidney is required to survive. In general, organs from living donors function better and for longer periods of time than those from donors who are deceased.
Overall, transplant success rates are very good. Transplants from deceased donors have an 85 to 90% success rate for the first year. That means that after one year, 85 to 90 out of every 100 transplanted kidneys are still functioning. Live donor transplants have a 90 to 95% success rate. Long-term success is good for people of all ages.
WKD 2012 was devoted to spreading the message about the importance of organ donation and kidney transplantation for people with ESRD.
Dialysis
Healthy kidneys clean blood and remove extra fluid in the form of urine. They also make substances that keep our body healthy. Dialysis replaces the blood cleaning functions when kidneys no longer work.
There are two types of dialysis: hemodialysis and peritoneal dialysis.
In hemodialysis, your blood is pumped through a dialysis machine to remove waste products and excess fluids. You are connected to the dialysis machine through a needle in a vein that is surgically enlarged (vascular access) or through a temporary plastic catheter placed in a vein. This allows blood to be removed from the body, circulate through the dialysis machine for cleansing, and then return to the body. Hemodialysis can be done at a dialysis center or at home. When done in a center, it is generally done three times a week and takes between three and five hours per session. Home dialysis is generally done three to seven times per week and takes between three and ten hours per session (often while sleeping).
Peritoneal dialysis is another form of dialysis used to remove waste products and excess water. It works on the same principle as hemodialysis, but your blood is cleaned while still inside your body rather than in a machine by adding clean fluid to your abdomen, letting it accumulate waste products from the blood and then draining it out. It is typically done at home. Some patients can perform peritoneal dialysis continuously while going about normal daily activities (continuous ambulatory peritoneal dialysis, CAPD)
INTRODUCTION
Dialysis and kidney transplantation are treatments for severe kidney failure, also called kidney (or renal) failure, stage 5 chronic kidney disease, and end-stage kidney (or renal) disease. There are two types of dialysis: hemodialysis and peritoneal dialysis.
When the kidneys are no longer working effectively, waste products, electrolytes, and fluid build-up in the blood. Dialysis takes over a portion of the function of the failing kidneys to remove the fluid and waste products. Kidney transplantation can even more completely take over the function of the failing kidneys.
This article discusses these therapies, including the advantages, disadvantages, and care required for kidney transplantation and dialysis. You and your family should discuss all of the options with your healthcare provider to make an informed decision.
WHEN WILL DIALYSIS OR KIDNEY TRANSPLANTATION BE NEEDED?
As the kidneys lose their ability to function, fluid, waste products, and electrolytes begin to build up in the blood. A kidney transplant should be performed or dialysis should begin before kidney disease has advanced to the point where life-threatening complications occur. This usually takes many months or years after kidney disease is first discovered, although sometimes severe kidney failure is discovered for the first time in people who were not previously known to have kidney disease. (See "Patient education: Chronic kidney disease (Beyond the Basics)".)
If you have advanced kidney disease and you plan to start dialysis, it is best to begin dialysis treatments while you still feel well and have only mild symptoms of kidney failure. Such symptoms include nausea, loss of appetite, loss of energy, vomiting, difficulty concentrating, and others. You and your doctor will decide when to begin dialysis after considering a number of factors, including your kidney function (as measured by blood and urine tests), overall health, and personal preferences. Most patients will have symptoms of kidney failure and thus generally plan to start dialysis when their kidney function is approximately 5 to 10 percent of normal.
KIDNEY TRANSPLANTATION
Kidney transplantation is considered the treatment of choice for many people with severe chronic kidney disease because quality of life and survival (life expectancy) are often better than in people who are treated with dialysis. However, there is a shortage of organs available for donation. Many people who are candidates for kidney transplantation are put on a transplant waiting list and require dialysis until a kidney is available.
A kidney can be transplanted from a relative, an unrelated person (such as a spouse or friend), or from a person who has died (deceased or cadaver donor); only one kidney is required to survive. In general, organs from living donors function better and for longer periods of time than those from donors who are deceased.
Some people with kidney failure are not candidates for a kidney transplant. Older age and severe heart or vascular disease may mean that it is safer to be treated with dialysis rather than undergo kidney transplantation. Other conditions that might prevent a person from being eligible for kidney transplantation include:
Some people with human immunodeficiency virus (HIV) infection may be eligible for kidney transplantation if their disease is well controlled.
People with other medical conditions are evaluated on a case-by-case basis to determine if kidney transplantation is an option.
Advantages — Kidney transplantation is the treatment of choice for many people with end-stage kidney disease. A successful kidney transplant can improve your quality of life and reduce your risk of dying. In addition, people who undergo kidney transplantation do not require hours of dialysis treatment. Ideally, patients who are eligible to get a kidney transplant do so before ever starting on dialysis.
Disadvantages — Kidney transplantation is a major surgical procedure that has risks both during and after the surgery. The risks of the surgery include infection, bleeding, and damage to the surrounding organs. Even death can occur, although this is very rare.
After kidney transplantation, you will be required to take medications and have frequent monitoring to minimize the chance of organ rejection; this must continue for your entire lifetime. The medications can have significant side effects, including increased risk of severe infections, diabetes, and some cancers.
HEMODIALYSIS
In hemodialysis, your blood is pumped through a dialysis machine to remove waste products and excess fluids. You are connected to the dialysis machine using a surgically created path called a vascular access, also known as a fistula or graft. Sometimes, a catheter inserted into a large vein in the neck is used for hemodialysis treatments, although it is better to have a fistula or graft. This allows blood to be removed from the body, circulate through the dialysis machine, and then return to the body.
Hemodialysis can be done at a dialysis center or at home. When done in a center, it is most commonly done three times a week and takes between three and five hours per session. In-center hemodialysis can also be done with an overnight treatment three times per week. Home dialysis is generally done three to six times per week and takes between 3 and 10 hours per session (sometimes while sleeping). More detailed information about hemodialysis is available separately. (See "Patient education: Hemodialysis (Beyond the Basics)".)
Advantages — Hemodialysis generally requires relatively few hours of treatment per day and does not usually include treatments every day. In-center hemodialysis does not require patients to learn much about the dialysis procedure itself, and a nurse or patient care technician takes care of getting access to the blood stream for treatments.
Disadvantages — Low blood pressure during treatments is the most common complication of hemodialysis and can be accompanied by lightheadedness, shortness of breath, abdominal cramps, nausea, or vomiting. Treatments and preventive measures are available for these potential problems. In addition, the access can cause a blood stream infection or get clogged up and need surgery or other procedures to open it up.
Many patients who receive hemodialysis in a center are either unable to work or choose not to work due to the time required for travel and the dialysis treatments. Sometimes, nighttime overnight hemodialysis treatments in a dialysis facility may make it easier to both work and have hemodialysis.
PERITONEAL DIALYSIS
Peritoneal dialysis is typically done at home. To perform peritoneal dialysis, the abdominal cavity is filled with dialysis fluid (called dialysate) through a catheter (a flexible tube). The catheter is surgically inserted into the abdomen near the umbilicus (belly button). (See "Patient education: Peritoneal dialysis (Beyond the Basics)".)
The fluid is held within the abdomen for a prescribed period of time (called a dwell), usually several hours. The lining of the abdominal cavity (the peritoneal lining) acts as a membrane to allow excess fluids and waste products to diffuse from the bloodstream into the dialysate. The used dialysate in the abdomen is then drained out and discarded. The abdominal cavity is then filled again with fresh dialysate solution. This process is called an exchange.
Peritoneal dialysis treatments may be done by hand four to five times during the day or by using a machine (called a cycler) while you sleep. Some people use a cycler at night and also do one or two exchanges during the day.
Advantages — Advantages of peritoneal dialysis compared with hemodialysis include more uninterrupted time for work, family, and social activities. Many people who use peritoneal dialysis are able to continue working, at least part time, especially if exchanges are done during sleep.
Disadvantages — People who use peritoneal dialysis must be able to understand how to set the equipment up and use their hands to connect and disconnect small tubes. If you cannot do this, a family or household member may be able to do it.
Disadvantages of peritoneal dialysis include an increased risk of hernia (weakening of the abdominal muscles) from the pressure of the fluid inside the abdominal cavity. In addition, you can gain weight, and you have an increased risk of infection at the catheter site or inside the abdomen (peritonitis), although this is quite rare.
WHICH THERAPY IS BEST FOR ME?
Kidney transplantation is the optimal treatment for most patients who do not have one of the reasons to be ineligible for transplant that were mentioned above (see 'Kidney transplantation' above). Patients who are not candidates for kidney transplantation or who must wait for a kidney can usually be treated with either hemodialysis or peritoneal dialysis.
Choosing between peritoneal dialysis and hemodialysis is a complex decision that is best made by you, your doctor, and often other family members or caregivers after careful consideration of a number of important factors. It seems that neither hemodialysis nor peritoneal dialysis have clear advantages over the other in terms of survival. The choice between the two types of dialysis is generally based upon other factors, including your preferences, home supports, and underlying medical problems. You should begin with the type of dialysis that you and your doctors think is best, although it is possible to switch to another type as circumstances and preferences change.
For example, hemodialysis involves rapid changes of the fluid balance in the body and cannot be tolerated by some patients. Some patients are not suitable candidates for kidney transplantation, while others may not have the home supports or abilities needed to do peritoneal dialysis. Your overall medical condition, personal preferences, and home situation are among the many factors that should be considered. It is possible to switch from one type of dialysis to the other if preferences or conditions change over time.
NOT STARTING DIALYSIS
Some people choose not to start dialysis at all. You and your family should discuss the risks and benefits of long-term dialysis with your doctors.
Most people with kidney disease who have no or few other chronic illnesses are encouraged to start dialysis or get a kidney transplant; the chance of having a high quality of life for an extended period of time is usually excellent. However, you may have compelling reasons for electing not to start dialysis; this is often due to advanced age and having other medical conditions that might limit long-term life expectancy that would not be prolonged by starting dialysis. Try to feel comfortable discussing your wishes with your family and healthcare team with the goals of death with dignity and life with quality.
Prevalence of CKD
About 1 in 10 people have some degree of CKD. It can develop at any age and various conditions can lead to CKD.
Kidney disease can affect people of all ages and races. African Americans, Hispanics, American Indians and people of South Asian origin (those from India, Bangladesh, Sri Lanka or Pakistan) have a higher risk of CKD. This risk is due in part to high rates of diabetes and high blood pressure in these communities.
CKD can occur at any age, but r becomes more common with increasing age and is more common in women. Although about half of people aged 75 or more have some degree of CKD, many of these people do not actually have diseases of their kidneys; they have normal ageing of their kidneys. Simple blood and urine tests can detect CKD and simple, low cost treatments can slow the progression of the disease, reduce the risk of associated heart attacks and strokes and improve quality of life.
Cost of CKD
The prevalence of kidney disease is increasing dramatically and the cost of treating this growing epidemic represents an enormous burden on healthcare systems worldwide. Even in high income countries, the very high cost of long term dialysis for increasing numbers of people is a problem. In low and middle income countries long term dialysis is unaffordable. The best hope for reducing the human and economic costs of chronic kidney disease and end-stage renal disease therefore lies in prevention, for the following reasons:
In developed countries, ESRD is a major cost driver for patients, their families and the taxpayer. Patients with ESRD require dialysis or kidney transplantation, which are highly costly and consume a sizeable portion of the health budget.
For instance:
In middle-income countries, access to life-saving therapies has progressively increased over the same period yet renal replacement therapy remains unaffordable for the majority of patients.
Developing countries, with a combined population of over 600 million people, cannot afford renal replacement at all—resulting in the death of over 1 million people annually from untreated kidney failure. Indeed, more than 80% of individuals receiving renal replacement therapy (RRT) live in the developed world because in developing countries it is largely unaffordable. In countries such as India and Pakistan, less than 10% of all patients who need it receive any kind of renal replacement therapy. In many African countries there is little or no access to RRT, meaning many people simply die. RRT is also used to treat acute kidney injuries where recovery of kidney function usually occurs if the patient can be kept alive by dialysis until that happens. The lack of available RRT results in the preventable deaths of many thousands of children with diarrheal diseases and women with complications of pregnancy in the developing world every year (see below). WKD 2013 was dedicated to spreading the message of the importance of acute kidney injury (AKI).
Examples of costs from other regions of the world: https://www.acad.emia.edu/3633811/Chronic_kidney_disease_global_dimension_and_perspectives
CKD in elderly people
About 1 in 10 people have some degree of CKD. It can develop at any age and various conditions can lead to CKD. It however becomes more common with increasing age. After the age of 40, kidney filtration begins to fall by approximately 1% per year. On top of the natural aging of the kidneys, many conditions which damage the kidneys are more common in older people including diabetes, high blood pressure and heart disease.
It is estimated that about one in five men and one in four women between the ages of 65 and 74, and half of people aged 75 or more have CKD. In short, the older you get the more likely you are to have some degree of kidney disease. This is important because CKD increases the risk of heart attack and stroke, and in some cases can progress to kidney failure requiring dialysis or transplantation. Regardless of your age, simple treatments can slow the progression of kidney disease, prevent complications and improve quality of life.
| S | M | T | W | T | F | S |
|---|---|---|---|---|---|---|
| 1 | 2 | |||||
| 3 | 4 | 5 | 6 | 7 | 8 | 9 |
| 10 | 11 | 12 | 13 | 14 | 15 | 16 |
| 17 | 18 | 19 | 20 | 21 | 22 | 23 |
| 24 | 25 | 26 | 27 | 28 | 29 | 30 |
| 31 |
Online: 8
Today: 507
Yesterday: 0
Week: 507
Month: 507
Year: 53798
Total: 339286
Dr. Md. Farhad Hasan Chowdhury, 219, Elephant Road, Dhaka.
hasanfarhad75@gmail.com
brabd.org@gmail.com
© Bangladesh Renal Association 2020
Developed by BDHOST